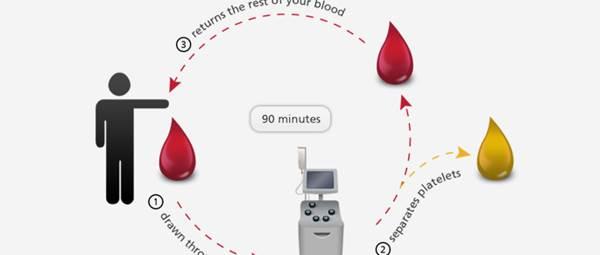
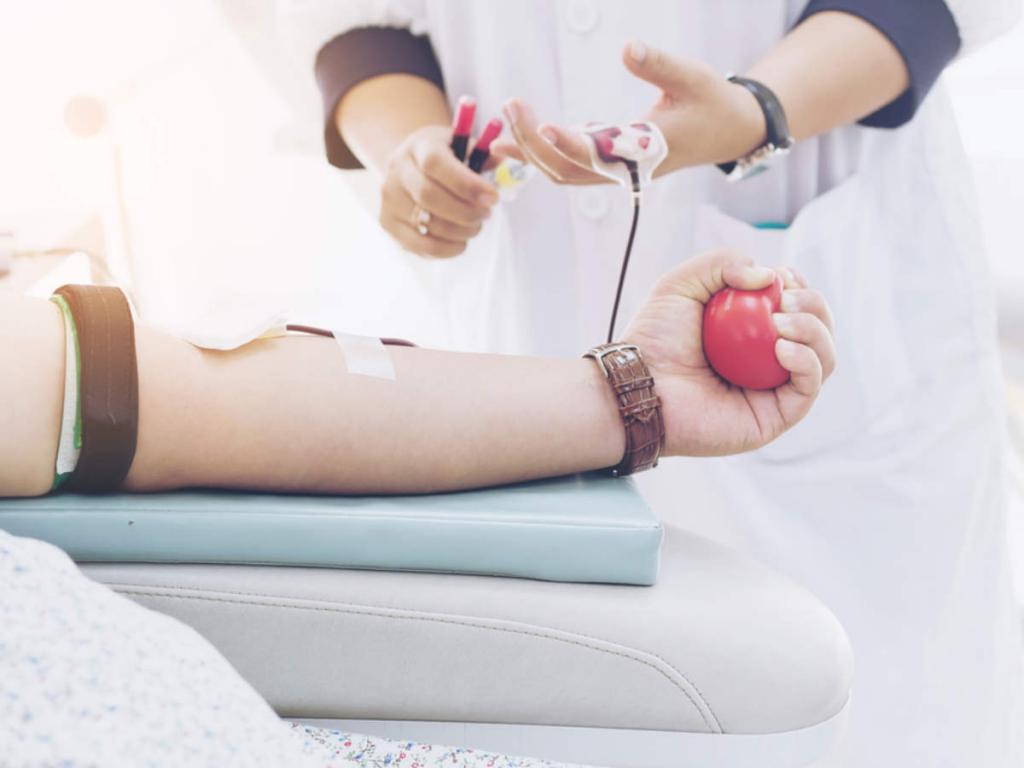
What kind of needle is used to draw plasma, if you please? Any needle will do, but a safety needle is preferable because it prevents accidental needle sticks. Needles used for blood donations must be thrown away after use.
It’s crucial to have all the right tools available when giving blood. Adherence to the blood-drawing protocol is of the utmost importance. If processes are not carried out appropriately and monitored thoroughly, infections may result.
Bạn đang xem: What Gauge Needle Is Used For Plasma Donation? Ultimate List
Particular tools are needed for the blood donation process. Adherence to the blood-drawing protocol is of the utmost importance. Infections could occur if procedures weren’t carried out correctly and monitored thoroughly.
What Is A Gauge Needle?
It’s important to get ready for a blood donation by making sure you have everything you need. When taking a patient’s blood, a specific protocol must be followed. Infections may occur if protocols are not followed and monitored closely.
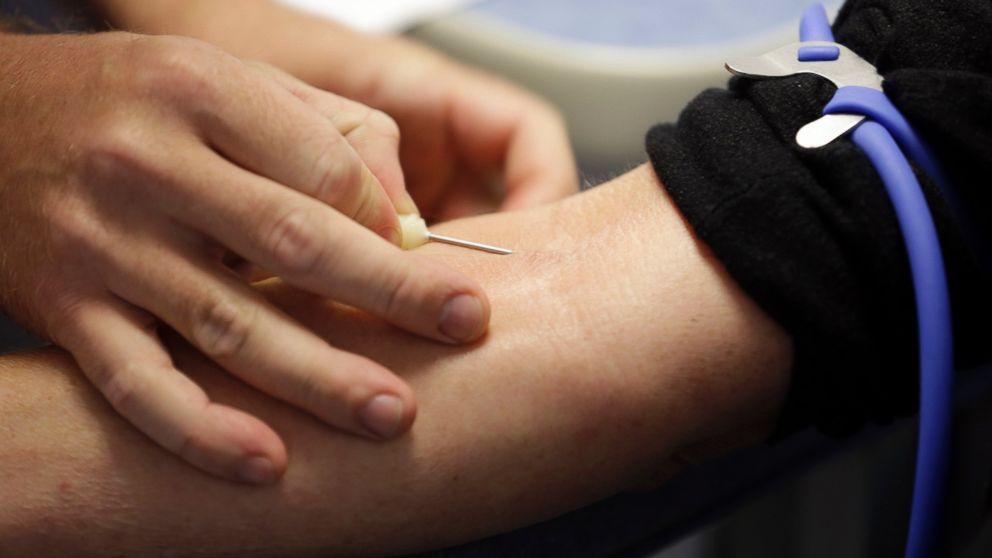
The Importance Behind Blood Donation
Donating blood is crucial for many reasons. The selflessness of blood donors has made modern medicine possible. The need for blood is increasing as the number of people in need and suffering from serious illnesses continues to climb. As long as the donor takes good care of themselves before, during, and after donating blood, there is little risk involved. If hospitals are going to be able to keep up with the growing demand for their services, more people need to donate blood. It has the added benefit of saving lives and restoring blood levels.
Lists Of Gauge Needles Used For Plasma Donations
Different needles with different gauges and diameters are used for blood donations. Blood flow and vein compatibility are taken into account before inserting each hand. Needles are used to inject medicine or draw blood from the body. Size and number of needles are related. Patients and blood donors are free to self-identify as adults or minors. All the information you need to know about needle gauges before giving blood is provided below. So, how big of a needle do you need to donate plasma?
18 gauge needle
Needles used for blood donations can be found in a variety of sizes and gauges. Before inserting either hand, doctors make sure there will be adequate blood flow and that the veins are compatible. Needles are used for a variety of medical procedures, including injecting medication and draining bodily fluids. The distance between each needle and its neighbor is proportional to its diameter. Individuals seeking medical care or donating blood have the right to choose whether or not to disclose their age. Following is a chart of needle gauges that can be used when giving blood. So, how big of a needle do you need to donate plasma?
21 gauge needle
There is a vast variety of needle sizes and gauges used in blood donation. This procedure can only be successful if the vein type and blood flow rate of the donor hand are a perfect match for the patient’s veins and hands. Needles are used to administer medication or remove fluids from the body. Needles can vary in length, and the two are connected. If a patient or donor questions their own legal eligibility, that decision rests with them. You can use one of the needles with the following gauges before giving blood. What size needle do you use if you want to give plasma?
22 gauge needle
Needles for blood donations come in a variety of diameters and gauges. Each hand is surgically placed into a vein with a blood flow rate that is suitable for that hand. A needle is a tool used for injecting medicine or drawing blood for laboratory analysis. Needles can range in size, with the larger ones typically having more of them. If a patient or donor is unwilling to reveal their age, such information will be kept confidential. The many needle gauges that can be used during the blood donation process are detailed below. How big of a needle is needed to extract plasma from a donor.
23 gauge needle
Needles used for blood donations can be found in a variety of sizes and gauges. Before inserting either hand, doctors make sure there will be adequate blood flow and that the veins are compatible. Needles are used for a variety of medical procedures, including injecting medication and draining bodily fluids. The distance between each needle and its neighbor is proportional to its diameter. Individuals seeking medical care or donating blood have the right to choose whether or not to disclose their age. Following is a chart of needle gauges that can be used when giving blood. When giving plasma, what size needle do you use?
Reasons For Securing A Gauge Needle To Be Used For Blood Donation
In procedures involving blood, it is essential to use a needle of the appropriate gauge. The health and safety of the patient and the donor must be prioritized at all times throughout a blood transfusion. If you intend to give blood, you should always have a needle on hand.
#1. Safety
At all times, people’s and patients’ health and safety should be the first priority. Donors should only use dependable needles of the highest quality. When giving an injection, they make sure the needle is clean, straight, and sterile for the patient’s protection.
#2. Accuracy
It is crucial that blood donations be made correctly. The standard of the technique and the needle used determine the outcome and patient’s reaction to it. Accuracy enhances output and decreases the likelihood of errors occurring in any procedure.
#3. To follow a procedure
Xem thêm : What Is Autologous Blood Donation? Facts You Need To Know
Keeping a needle close at hand is normal practice in the scientific community. There is a lengthy process involved in accepting a blood donation. Certain needles are required for use with specific blood treatments.
#4. To prevent clotting
It is essential that blood donors adhere to all procedures precisely. Needles that have been recently cleaned and sterilized are crucial in blood transfusions because they help prevent dangerous consequences like blood clots and infections.
#5. To provide significant cost savings
For the sake of the patient or blood donor, it is crucial that the gauge needle be safely stored before usage. This tactic is useful for people and businesses since it reduces costs and saves time. Taking care of one’s health is similar to insuring one’s wealth.
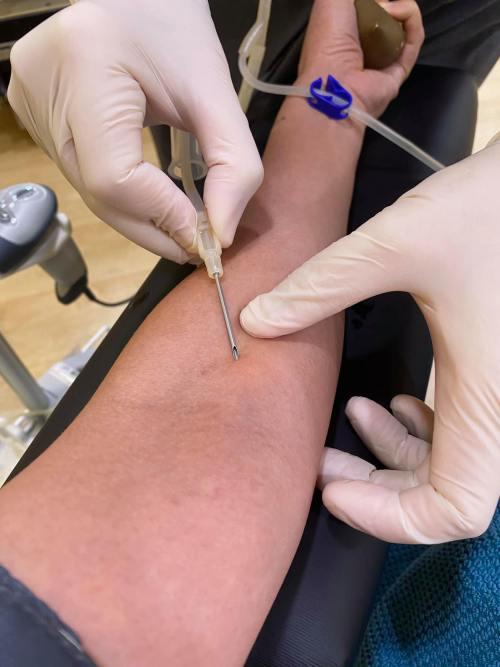
Background information on venepuncture for blood donation
Blood banks use a wide variety of methods to prevent the spread of disease through donor blood. Donors should ideally come from communities with low risks of bloodborne disease infection, such as those who give blood voluntarily and without compensation and those who have never used intravenous drugs. Additional screening questions (which may vary by area) may be asked of donors to help identify those who are at a higher risk of contracting an infection. Phlebotomists have to be very careful to follow detailed inclusion and exclusion criteria for donors. Donated blood is screened for regionally common diseases before it is used for therapeutic purposes.
In order to prevent the spread of disease, blood banks employ a variety of measures to screen donors and process their donations. Donors should ideally come from communities with low risks of bloodborne disease infection, such as those who give blood voluntarily and without compensation and those who have never used intravenous drugs. If further information is needed to determine which donors are at a higher risk of developing a disease, additional screening questions may be asked of donors (these questions may differ according on the region). Phlebotomists have a responsibility to adhere to all donor eligibility requirements. Donated blood is tested for locally-endemic illnesses before it is used therapeutically, which is the third safety step in place.
It is vital to put an effective antiseptic on the donor’s arms before collecting blood since skin flora is a common source of illness. If blood components were contaminated with foreign pathogens or other things, transfusional therapy could have harmful effects. Despite the lack of conclusive trials, a mixture of 2% chlorhexidine gluconate and 70% isopropyl alcohol is the preferred technique of skin antisepsis for blood donation, to be applied for 30 seconds, followed by 30 seconds of drying time.
Donations of blood should only be collected by medical professionals working for a blood transfusion service.
Minimum requirements for venepuncture for blood donation
Guidelines for closed systems are outlined in Chapter 3, and it is advised that you read Chapter 2 first before planning, locating, and implementing infection prevention and control measures. In addition, a blood donation collection system should include the following features.
- Donation equipment must be regularly checked, calibrated, maintained, and repaired. A few examples are blood pressure monitors, scales, donor couches or chairs, blood collection monitors or mixers, blood bag tube sealers, blood transport boxes, and blood bank refrigerators.
- Donation and processing centers for blood need furniture and equipment with smooth, easily cleaned surfaces (e.g. vinyl rather than fabric). Containers used to transport supplies and specimens should be sterilizable using disinfectants like sodium hypochlorite bleach solutions.
- Fabric and textile carriers can be machine-washed when they get dirty. Use a closed collection system consisting of a sterile blood collection bag with anticoagulant, a linked tube, and a needle.
- The use of diversion pouches in blood collection containers helps reduce the risk of contamination from skin bacteria and skin cores. When drawing blood for hemoglobin testing, it’s important to use a sterile, single-use lancet to prevent contamination.
Workers should not be exposed to respiratory illnesses by waiting in a waiting room that is not the collection area.
It’s important that both permanent and temporary donation facilities for blood share the same environmental safety standards.
Before a blood donation
To ensure the safety and efficacy of blood transfusions, the World Health Organization (WHO) has established pre-donation protocols. Donating blood is an act of altruism that should not be motivated by rewards of any kind. Donors of blood should be selected in accordance with federal regulations.
Before a blood donation may be made, the following must be completed:
- A prospective donor should be provided with pre-donation blood donation information, advice, and counseling;
- Investigate the donor’s medical history and any risky behaviors they may have engaged in. new and current medication use; -the presence or absence of a chronic infection; -the presence or absence of a history of prolonged bleeding or a diagnosis of bleeding problems; -the presence or absence of a history of previous donations; -the presence or absence of a history of a mastectomy; and -the (blood should be taken from the arm opposite the site of surgery).
- Before any treatments are done, a donor’s health should be evaluated, including their weight, blood pressure, and the presence of infection or scarring at prospective sites.
- Donors should be provided with fluids to ensure they don’t become dehydrated after giving blood.
- In accordance with local regulations, the individual must offer their written consent.
Practical guidance on venepuncture for blood donation
Collecting blood
Donating blood can also make use of the techniques outlined in Chapter 2 (such as hand hygiene and glove use), provided that doing so is safe and effective.
Step1. Identify donor and label blood collection bag and test tubes
- Find out the donor’s complete name.
- Before submitting a blood sample, make sure that: -the right patient name and number are on the blood collection bag, satellite bags, sample tubes, and donor records; -the labels on the blood collection bag, satellite bags, sample tubes, and donor records are correct.
Step 2. Select the vein
- In the antecubital fossa, you should search for a large, healthy vein that is devoid of scarring or other skin defects.
- Inflated tourniquets or cuffs can help medical personnel concentrate on the vein (40-60 mm Hg).
- A large number of back-and-forth motions of the donor’s hand are required.
- Take off the tourniquet or other pressure device from the vein before you start cleaning the skin.
Step 3. Disinfect the skin
- Use sterile water and paper towels to clean the venepuncture site if it seems unclean.
- Just follow these brief, simple instructions. Make sure to give the disinfectant at least 30 seconds to soak into your skin after a thorough application. Wait at least 30 seconds after administering the disinfectant to allow the area to dry thoroughly.
- A solution of 70% isopropyl alcohol and chlorhexidine gluconate can be made in less than two minutes if you don’t have access to any. First, apply a disinfectant containing 70% isopropyl alcohol and let it dry for about 30 seconds; -the skin should be in direct contact with the disinfectant for at least 30 seconds.
- After disinfecting the area, you should not touch the venepuncture site.
Step 4. Perform the venepuncture
Xem thêm : How To Organize A Donation Drive? Simple Tips
In Section 2.2.3, Step 6, you will learn how to properly insert the needle and make a clean incision. The following considerations should be kept in mind when you make your decision about whether or not to become a blood donor.
- The needle that comes with the blood collection bag should typically be a 16-gauge needle (see Table 3.1 in Chapter 3). Needle caps and safety needles should be removed rather than recapped after use (step 6 below).
- Make a fist and slowly open and close it once every 10 to 12 seconds.
- If blood flow has been restored after two minutes, you can remove the tourniquet.
Step 5. Monitor the donor and the donated unit
- The donor and the injection location should be under constant surveillance during the whole donation process. The needle may need to be retrieved and reinserted if it is placed too deeply into the vein, causing a haematoma at the injection site. Perspiring, pallor, and reports of dizziness are all indicators of fainting that may appear minutes or hours before the actual loss of consciousness.
- Donors should use a hand mixer or a continually running mechanical mixer to gently combine the blood and anticoagulant once every 30 seconds.
Step 6. Remove the needle and collect samples
- Sterilized shears can be used to remove the needle.
- In order to conduct tests in a lab, it is necessary to collect and analyze blood samples.
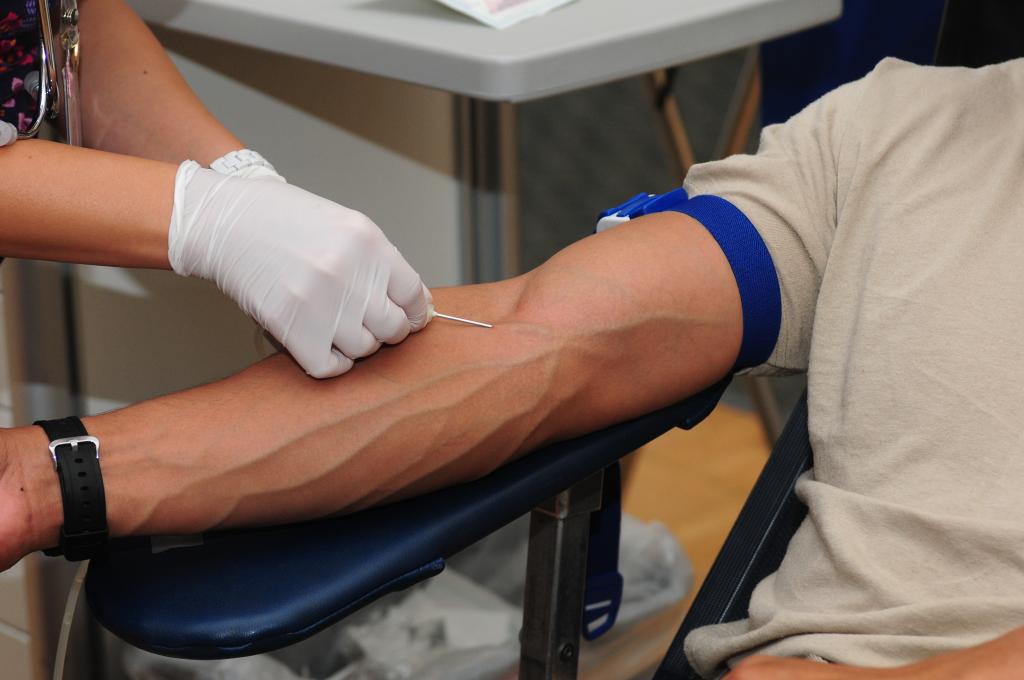
After a blood donation
Donor care
When you’re done drawing blood, do the following:
- Do not rush them; give them a moment to collect themselves before you answer;
- Apply a bandage to the venepuncture site even if it is not bleeding. It is imperative that additional pressure be applied if there is any sign of bleeding.
- slowly stand up and inquire about the donor’s health;
- Make sure the donor doesn’t feel faint or have a dip in blood pressure before allowing them to leave the donation room.
- Invite the donor to a cocktail reception.
Blood unit and samples
- Using the blood center’s recommended procedures and the product’s specifications, store the blood unit in a container designed for long-term storage.
- As such, taking a blood sample and transporting it to the lab is a serious endeavor that calls for meticulous record-keeping, careful storage, and a leak-proof, secure transit container.
Adverse events in blood donation
It’s important to keep an eye out for danger and train for a quick response.
Does Donating Plasma Hurt
Indeed, it is painful to experience. Your arm looks like it was pricked with a really big needle. The answer lies in the degree to which it bothers you. Donating blood or getting a flu shot are two alternatives that are not vastly different from this method.
The process of donating plasma is not simple, but if you can get through it, you should be fine. Upon having the needle placed into your arm, you will experience no pain.
The insertion of the needle by the phlebotomist is often the most important part of the procedure. No doubt you’ve had injections ranging from completely painless to extremely agonizing. The agony is not caused by the needle itself, but by the hand that holds it.
If you have a negative experience giving blood, it’s probably the fault of the phlebotomist and not the technique itself. You may wish to choose a more seasoned specialist the second time around, if you are not afraid of needles and shots.
In addition, consider the veins in your body and the types they are. Your veins may be too tiny or obscured for a less invasive procedure. The needle might not go in all the way, or more than one vein might be missed (infiltration). It may be necessary to prick the skin more than once or to reposition the needle in order to reach a vein.
There’s a potential you won’t be able to donate blood even if they succeed in performing the surgery due of discomfort or other after effects. Because “plumped up” veins facilitate blood donation, maintaining adequate fluid intake is critical. Before making your first donation, read this post for some useful tips.
Some people may also feel uneasy about the screening process, which involves getting their finger poked, as part of the procedure for donating plasma. Donors say it hurts more than the venipuncture, despite the fact that the prick is much smaller (needle stick).
You should realize that the act of donating will not affect your body in any way. A needle puncture generates actual, though fleeting, pain. Not bad, thinking about the money you can make by donating plasma.
Donations can have unintended consequences that are unpleasant at best and even damaging at worst for the giver and their loved ones. They’re not common, but they’re also not impossible. This post contains further information about possible side effects, so be sure to read it.
Conclusion
Learning how to properly gauge a needle will help you become a more knowledgeable and conscientious plasma donor. Your health and safety before, during, and after giving blood may be addressed in this guide.
A 2016 percentage (percent 2C percent 20below) is preferred over a capped percentage of the population.
Nguồn: https://spasifikmag.com
Danh mục: Health